How Can AI Support The Use Of TrueBeam Radiotherapy?
Radiotherapy has come a long way since it was first used to treat cancer around the turn of the 20th century. Enhancements in technology, increased knowledge of radiation and the benefits of decades of medical research have enabled treatments to be far more effective.
Among the great strides forward was the invention of stereotactic radiosurgery. This technique and the term itself were both devised by Swedish neuroscientist Lars Leksell in the 1960s. His great innovation was Gamma Knife, a device still very much in use today.
The aim of the Gamma Knife, as well as other devices that offer stereotactic radiosurgery, was to concentrate beams of very intense radiation with great precision on specific areas. This had its most obvious use when treating brain tumours. The benefits were as follows:
- A high dosage could be accurately aimed at a small tumour to help shrink it effectively
- The intensity of the beam meant the dose could be delivered sooner, making sessions and the course of treatment shorter
- The precision not only meant the target area could be hit accurately, but the exposure of healthy tissue surrounding the tumour to radiation could be minimised, limiting the side effects.
These attributes made the Gamma knife and other stereotactic radiotherapy devices extremely effective in dealing with some of the most awkwardly located cancers.
Brain cancer is a prime example of tumours in a sensitive location, but there are other instances in which minimising exposure to sensitive organs around the body is highly beneficial.
How Has Stereotactic Radiosurgery Advanced?
The development of stereotactic radiotherapy has been advanced by a series of further innovations:
- Refinements to the Gamma Knife
- The development of other devices and technology, such as Truebeam Radiotherapy
- The use of improved scanning technology to guide the devices, including 3D scans
In addition to these, artificial intelligence (AI) is now starting to make its presence felt.
The use of AI across many areas of society and the economy is hotly debated, but it is already proving very useful in oncology, not least in diagnostics, as it has proved very effective in spotting signs of disease in scans.
However, it has other uses as well and one of those is in assisting advanced technologies such as TrueBeam.
What Is TrueBeam Radiotherapy?
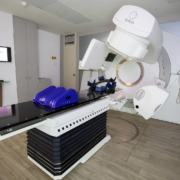
The TrueBeam system uses a hybrid linear accelerator to produce the beams of radiation that are then delivered with pinpoint accuracy to the target area.
It is aided by several advanced image guidance systems and uses a digital platform, deploying the most sophisticated and complex technology with the goal of delivering radiation to the tumour with unparalleled precision.
Another feature of the device is the capacity to modulate the radiation beam, which means various dosages and intensities of radiation can be aimed at different areas on the tumour.
This makes it advanced enough on its own, but the use of AI can take things further. All over the world, it is being used to aid TrueBeam.
How Has AI Been Used To Assist TrueBeam?
A recent example that made a few headlines was that of the AI-supported TrueBeam system now in use in the Aga Khan University Hospital in Kenya, Business Day reported.
The AI-assisted treatment planning is combined with motion tracking and real-time imaging to direct the beams with extreme accuracy levels. As well as being more precise, it is halving the average treatment session time from 20 minutes to ten.
Commenting on the use of the AI-backed TrueBeam system, the hospital’s head of radiotherapy, Dr Angela Waweru, said: “This allows us to treat tumours with unmatched accuracy and minimise damage to nearby organs, resulting in fewer side effects and faster recovery.”
Other features include synchronised treatment using motion management technology that can adjust the delivery of the radiation to tumours around the lungs, which move as the patient breathes.
This means that although the position of the tumour will vary, the machine will anticipate this and ensure it is continually directing the radiation at the target location.
Since the system was installed at the hospital last year, around 400 patients have been treated with it.
The provision of TrueBeam is particularly significant in Africa, where advanced cancer facilities are rare, but it is still at the cutting edge here in Europe, even alongside all the other modern technology and expertise that is in place.
How Can We Establish The Best Stereotactic Treatment Method For You?
If you need stereotactic radiosurgery, we can provide it using the most sophisticated methods available, be it TrueBeam, a Gamma Knife or any other means of delivery.
In consultation with our expert staff, we can establish both the right treatment methods and schedule to suit your particular circumstances and the specific details of your diagnosis, ensuring the best possible treatment to maximise the prospect of the best outcome.
Learn more about our advanced stereotactic radiosurgery treatments for different cancers on the Amethyst Group website.